 This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.ĭata Availability: This research was conducted using administrative claims data from Alabama Medicaid that includes PHI, which we accessed through a research contract with Alabama Medicaid. Received: NovemAccepted: JPublished: June 26, 2023Ĭopyright: © 2023 Sen et al. PLoS ONE 18(6):Įditor: Kevin Lu, University of South Carolina, UNITED STATES (2023) Telehealth use among pediatric Alabama Medicaid enrollees, March-December 2020: Variations by race/ethnicity & place of residence. This study’s findings suggest that attention needs to be paid to addressing race/ethnicity disparities in accessing telehealth services.Ĭitation: Sen B, Rahim MJ, McDougal J, Sharma P, Yang N, Brisendine A, et al. Pediatric enrollees in large rural areas and isolated areas were significantly less likely (IRR: 0.90 for both, p<0.05) to use telehealth than those in urban areas. This study employed a multivariate Poisson mixed-effects model with robust error variance to obtain differences in telehealth utilization and found that Non-Hispanic Black children were 80% as likely, Hispanic children were 55% as likely, and Asian Children were 46% as likely to have used telehealth compared to Non-Hispanic White children. There were 637,792 pediatric enrollees in the Alabama Medicaid program during the study period, and 16.9% of them had used telehealth to meet healthcare needs. 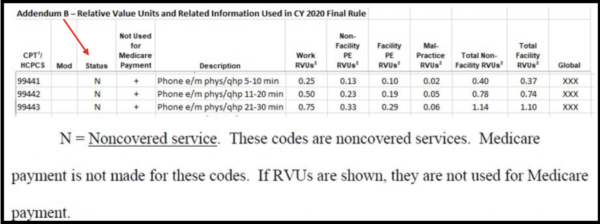
This retrospective observational study examined Alabama Medicaid claims data from March to December 2020 for enrollees less than 19 years. The study investigated telehealth use variation by race/ethnicity and place of residence for the pediatric enrollees of the Alabama Medicaid program. The Center for Connected Health Policy is tracking COVID-19 Related State Actions.During the early days and months of the COVID-19 pandemic, healthcare facilities experienced a slump in non-COVID-related visits, and there was an increasing interest in telehealth to deliver healthcare services for adult and pediatric patients. 
The AAFP recommends reaching out to your provider relations representatives or Medicare Administrative Contractors (MACs) to verify policies. Similarly, Medicaid policies are established at the state-level. 
Self-funded plans can develop their own policies and may opt out of some cost-sharing waivers. Cost-sharing waivers may not be applied to claims that do not include an appropriate COVID-19 ICD-10 diagnosis code. Coding guidance can be found on the CDC website. 
Use the POS used for typical services.ĬOVID-19-related services should be assigned the appropriate COVID-19 ICD-10 diagnosis code. There are no COVID-19-specific POS or modifier requirements for virtual check-ins or e-visits. However, Medicare will not cover the beneficiary’s cost-sharing and the service will be paid as usual. Physicians may elect to waive cost-sharing for Medicare beneficiaries. Virtual check-ins and e-visits must technically be initiated by a patient however, physicians and other providers may need to educate beneficiaries on the availability of the service prior to patient initiation.Īs noted above, most payers are waiving cost-sharing for virtual check-ins and e-visits. Beginning March 1 and for the duration of the public health emergency, patient consent may be obtained either before or at the time of service. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
